The DCN number is located on the remittance advice. This number must be used with adjustment/cancellation bills.
.
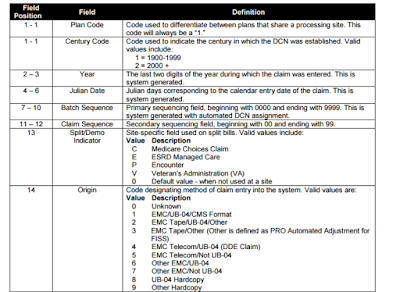


CLAIMS PROCESSING
A brief description of claims processing methods follows. All paper submitted claims are assigned a unique Document Control Number (DCN). The DCN identifies and tracks claims as they move through the claims processing system. This number contains the Julian date, which indicates the date the claim was received. It monitors timely submission of a claim.
Document Control Numbers are composed of 11 digits:
2-digit plan year
3-digit Julian date
2-digit BCBSTX reel identification
4-digit sequential number
Claims entering the system are processed on a line-by-line basis except for inpatient claims. Inpatient claims are processed on a whole-claim basis. Each claim is subjected to a comprehensive series of checkpoints called edits. These edits verify and validate all claim information to determine if the claim should be paid, denied or pended for manual review.
You are responsible for all claims submitted with your Provider number, regardless of who completed the claim. If you use a billing service you must help ensure that your claims are submitted properly.
Note: Entities submitting claims for services rendered by a Healthcare Provider are subject to Texas HHSC suspension if they submit claims for a Provider who is suspended from HHSC.

